“Yamma dummarung” the sign reads.
Welcome to the land of the three rivers. Welcome to Wiradjuri country.
It’s the first thing you see as you walk through any entranceway here, a very special campus of sorts in the centre of Wagga Wagga’s health district. It’s somehow fitting that the Riverina Medical and Dental Aboriginal Corporation – or RivMed, as it’s known to locals – was founded, and is still rooted in, a family home; family is at the heart of what they do, and everyone is greeted as kin.
Yandarra, a Wiradjuri word that means “coming together”, captures the essence of RivMed, an Aboriginal community-controlled health service that was established by a dedicated group of Elders some 30 years ago. These lands have, for tens of thousands of years, been a meeting place for the Wiradjuri, the people of the three rivers, and after British invasion it became a major resettlement community.

“They took them and put them all on the missions, and then they decided to move them off the missions and put them into towns,” explains RivMed CEO Tangerene Ingram, a Wiradjuri woman from the community of Brungle between Tumut and Gundagai, with a wry smile. “We have so many different nations living here.”
Ingram gestures at a map of Aboriginal nations as she traces the history of this town on the Murrumbidjeri, or Murrumbidgee, one of three rivers that give the Wiradjuri their name. Such maps are displayed prominently across RivMed, a celebration of and commitment to belonging.

“It’s not just the medical needs that are being met, and the dental needs, it’s also a meeting place,” explains Ingram of what sets RivMed apart. “Because it’s such a culturally safe space, you do feel comfortable. You go there, you see family, you see people you know, you see the Aboriginal person at the counter, it’s that type of service.”
Copies of the Koori Mail and photo albums celebrating events including the annual Yandarra health promotion festival are scattered throughout the waiting room of the Valda Weldon Primary Health Care Centre, named for Aunty Val, one of RivMed’s indomitable founders, whose portrait looks out over the glass doors.

RivMed Clinic Reception – Photo Credit: Amy Coopes
The television in the corner broadcasts Aboriginal Health TV (“We didn’t want to show mainstream,” says Ingram). A whiteboard next to the reception desk advertises community events: women’s cooking classes top this week’s schedule.
A tongue-in-cheek artwork depicting nunay ngurruway (bad choice) and marang ngurruway (good choice) has pride of place, with the latter panels featuring the preparation and hunting of traditional foods and a group of Wiradjuri women in ceremonial dress lifting weights around a stereo. ‘It’s your choice to be healthy’ the artwork states.

Though it retains a homely, familial warmth, RivMed has come a long way from humble beginnings in a house near the Wagga Wagga Base Hospital with just a handful of medical and dental staff. It’s now a thriving multidisciplinary service with some 6,000 clients and will soon boast almost 90 staff spanning the region, from Narrandera, Griffith and Leeton through Cootamundra and Brungle right down to Albury on the Victorian border.
“There’s a lot of things happening for RivMed,” says Ingram.
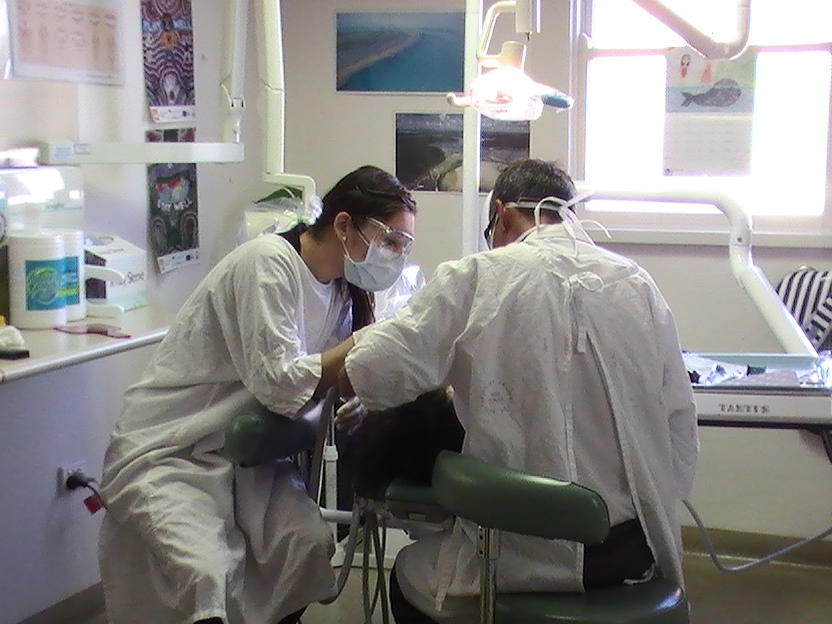
Families in focus
Ingram, whose background spans correctional services, health, social and emotional wellbeing and child protection and welfare, has overseen a remarkable expansion at RivMed in recent years, with a focus on at-risk children and families. She is ambitious and unapologetic about pushing the boundaries, with pride in the service’s work that is both boundless and infectious.
RivMed is one of the only services in regional NSW to offer a strengths-based, in-home program known as Functional Family Therapy (FFT), an early intervention targeting vulnerable families whose children are at risk of being taken into care due to issues ranging from substance use, domestic violence and trauma, through to squalor, grief and loss.
“The therapist goes into the home, and they start at the point at which the family is,” explains program manager Felix Machiridze, a former journalist who fled Zimbabwe as a refugee and has retrained in social work as part of his recovery.
“There is no top-down kind of approach, we say the family itself are the experts of their own issues, but what we try to do is to make the family see these issues in a different way.” – Felix Machiridze, Social Worker

Not every family in the program is Indigenous, but Machiridze says it resonates for Aboriginal people because it focuses on collective responsibility, inherent strengths, and social capital. In the two years it has been running, just one family out of 100 has needed to repeat the program, and it is such a success RivMed has hired staff in Albury, Narrandera and Cootamundra to extend its reach.
In a major win for the service – and a precedent that will now be rolled out statewide – RivMed convinced the NSW Government to broaden the referrals pathway so that it is not only Family and Community Services (FACS) and the Department of Communities and Justice that can refer families to the program. Instead, RivMed’s GPs and other staff, as well as the Family Referral Service, also will be able to direct families into the program.
“We have found for some families, especially most Aboriginal families, because of historical issues they do not want to do through the FACS pathway. They would rather not participate where FACS is concerned” says Machiridze.

In addition to FFT, RivMed runs an intensive 18-week family-based services initiative for Aboriginal families at risk and has been funded by FACS to offer two-year preservation and restoration programs working with families whose children have been or are at risk of being removed, with the aim of supporting a reunion or keeping a family intact. The project will have staff in Griffith, Narrandera and Leeton.
Following five years of lobbying, RivMed has just secured accreditation to offer out-of-home care to Aboriginal children, something of which Ingram is particularly proud.
“RivMed has always looked at the social and emotional wellbeing of the whole of the family,” she says. “Now we can take care of the health side, whether it’s the mental health, the drug and alcohol, your general GP health needs, to what’s happening with the family in terms of child protection… It’s a whole package, and we’re growing.”

Charting community need
Almost as swiftly as they move into a new building, RivMed outgrows it, such is the demand for services. The dentist needs another chair, there aren’t enough consult rooms for the busy roster of GPs, specialists, allied and mental health staff, and the clinic will soon have its very own in-house pathology lab on site. They have a clinic at Brungle, between Gundagai and Tumut, and have been involved in talks about supporting the Narrandera Aboriginal community with their health needs. Some 6,000 people are on the RivMed books.
Everything they do at RivMed is carefully calibrated to community need. They are one of four AMSs participating in the Sax institute’s longitudinal SEARCH study looking at the health and wellbeing of Aboriginal children, and their focus on vulnerable children arises directly from this research. According to the data, the most disadvantaged child in these populations are boys aged between three and nine who are in foster care, Ingram says.
“It’s really making us look at the program and how we can work better with our families.” – Tangerene Ingram, RivMed CEO

Food security has also emerged as a major pressure point for local people in the Sax study, particularly for people who “live out in the suburbs and can’t get into town because they don’t have the money, or mum’s on a pension, how can they get access”, Ingram says.
“If you’ve only got ten dollars you’re not going to be able to purchase meat and your veggies or whatever, they are going to go and spend it on a big heap of chips and Devon or bread because that’s going to feed all the kids.” – Tangerene Ingram, RivMed CEO
The service works with Oz Harvest locally to give out fresh food at the clinic and is leading discussions with local NGOs including St Vincent de Paul and the Salvation Army on how to better support the community.

As part of a multi-AMS consortium in the region caring for those with chronic conditions, RivMed administers Integrated Team Care Program funding, providing transport to specialist consults, accommodation if required, even paying for appointments. In the few years it has been running, this program has been a huge success. A dedicated Aboriginal Health Worker, Patrick Sagigi, does chronic care outreach into the community, following up with patients after procedures and operations. A beaming, burly young Torres Strait Islander who exudes bonhomie, he grins as we talk about his work.
Aboriginal Health Workers are what makes the service special, according to Practice Manager Jane Kearnes, who started her life at RivMed working on reception and now oversees the day to day operations of the medical clinic.

Because they are known in the community, and for our community a face that they know in our service, it makes them more comfortable… They have really important roles within the organization” says Kearnes.
Natalie Smith has been an Aboriginal Health Worker at RivMed for almost ten years and speaks with passion about her work.
“It’s so important to have us, [to overcome] that barrier between our clients and the GPs. Our clients are happier to engage with us, and for us to go out into the community and find them, we’ve got more knowledge of the communities, the families,” she says.

Navigating the mainstream
Helping people navigate the mainstream health system is an essential part of her job, and something thrown into sharp relief by the death of Naomi Williams, 27, and her unborn baby at Tumut Hospital in 2016. The incident sent shockwaves through the RivMed community, with many local people, including Ingram, calling Williams family. “It really impacted on this community,” she says.
An inquest into the young mother’s death found “clear and ongoing inadequacies” in her care and called on the Local Health District to improve the cultural safety of its service by bolstering its Indigenous workforce and addressing implicit bias. Ingram has been in talks with the district on “how we can work better together, and service the smaller communities as well”.
Smith will accompany clients who need escalation to hospital and stay with them until they are triaged, seen by a doctor, and handed over to the care of the Aboriginal Liaison. She will ensure they understand what is going on and feel safe before she returns to the clinic.
Trust of mainstream services is an ongoing issue for the community. Of the four services participating in the SEARCH study, RivMed has the highest percentage rate for mental health presentations to hospital, and Smith says these largely occur after hours and on weekends when RivMed’s team are not available.

“I think it’s our clients not wanting to access mainstream services, not having a familiar face from our community in the services,” she says. “For us, it’s about looking at what we can put in place to try and fix that for our community.”
Down the hall, Annika Honeysett’s rooms are a hive of activity, mums with prams exchanging news while their babies squawk happily. Honeysett is the AHW attached to the maternal and child health team, working closely with the midwife and shared care GPs to care for expectant and postpartum mums.
“I love it, especially when you see a mum from when they first come in to when they bring in the babies,” says Honeysett, who has been at RivMed for four years and trained as an AHW “to help my family and my community”.
“If we don’t help our community, nothing gets done… They see our faces and they know who we are out in the community. That makes them feel comfortable, safe” she says.

Vignettes
Natalie Smith, AHW and SEARCH Research Officer
Wagga born and bred and a dyed-in-the-wool community advocate, Wiradjuri woman Natalie Smith has been an AHW at RivMed for almost 10 years and says she can’t imagine doing anything else. “I’d had no experience whatsoever in health, and I had no idea what I was getting myself into, but I love it and I’m still here,” she says. “[I love] our community, working with our community, improving the health of our community.” Smith is one of a small, tight-knit team of AHWs who keep RivMed’s clinical, dental and family services operations humming. She works closely with the GPs, following up patients in the community, triaging drop-ins to the clinic and assisting with high school health checks, as well as collecting and collating data for the SEARCH study. When patients have to go across to the Wagga Wagga Base Hospital she will go with them to ensure they are properly handed over and understand what is going on. “It’s about trying to stop the barrier between the client and mainstream, the client understanding what the doctors are telling them, because that is what our biggest problem is.”

Annika Honeysett, AHW, Maternal and Child Health
As an AHW attached to the maternal and child health team, Ngiyampaa woman Annika Honeysett has a unique connection with RivMed’s growing families. She will see expectant mothers from early pregnancy through to delivery, and do baby checks and immunisations once their little ones arrive. “I love it, especially when you see a mum from when they first come in to when they bring in the babies,” she says. Honeysett provides all the antenatal care a midwife can, charting heights, weights, kidney function and blood sugars, but it’s the ongoing relationship, and that trust and understanding that is so tangible in what she does. “They see our faces and they know who we are out in the community. That makes them feel comfortable, safe.”

This article was written by Amy Coopes, on behalf of Croakey Professional Services. It was sponsored by The Aboriginal Health and Medical Research Council (AH&MRC) of NSW, which had final say over the content.
Croakey Professional Services help generate funds to sustain our public interest journalism activities and also aim to provide a useful service to our readers. To find out more about the range of services on offer, see here.










